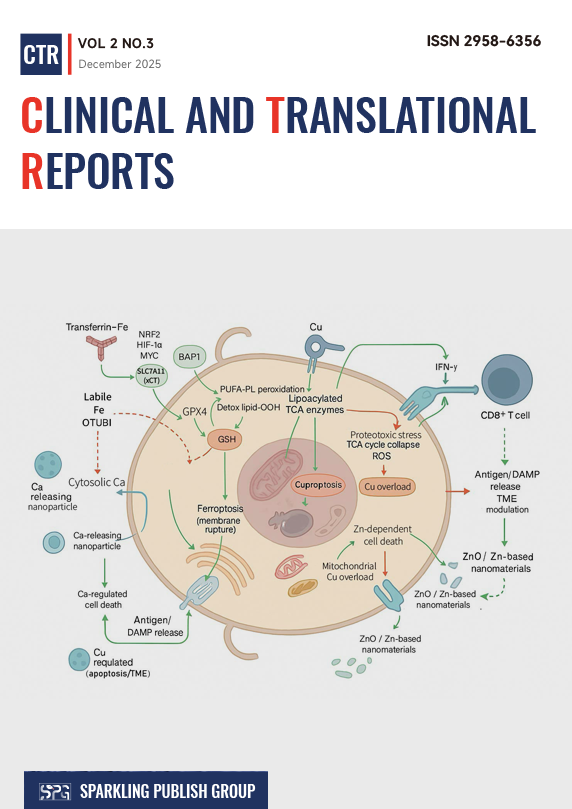
The tumor microenvironment (TME) is an ecosystem in which malignant cells co-evolve with immune, stromal, vascular, neural, and microbial components. Rather than acting in isolation, these compartments communicate through ligand-receptor signaling, direct contact, extracellular vesicles, extracellular matrix (ECM) remodeling, and metabolic exchange. This interaction network determines immune surveillance versus immune escape, governs invasion routes such as perivascular and perineural dissemination, and sets the threshold for therapy response and resistance. Single-cell and spatial omics studies emphasize the functionally reversible nature of specific microenvironments, while mechanistic work has exposed actionable coupling between tumor metabolism and myeloid polarization, fibroblast education, platelet-mediated metastatic priming, and vascular barrier functions. This review synthesizes the mechanistic axes of TME crosstalk, emphasize spatial and metabolic logic as organizing principles, discuss methodological strengths and pitfalls, and outline therapeutic strategies that target interactions rather than single cell types.
1. De Visser KE, Joyce JA. The evolving tumor microenvironment: From cancer initiation to metastatic outgrowth. Cancer cell. 2023;41(3):374-403. http://dx.doi.org/10.1016/j.ccell.2023.02.016
2. Althobiti MM. Tumor Microenvironment-Different Cells and Functions in the Metastasis and Progression of Cancer. International Journal of Pharmaceutical Investigation. 2025;15(1). http://dx.doi.org/10.5530/jphi.20250002
3. Dzobo K, Dandara C. The Extracellular Matrix: Its Composition, Function, Remodeling, and Role in Tumorigenesis. Biomimetics (Basel, Switzerland). 2023;8(2). http://dx.doi.org/10.3390/biomimetics8020146
4. Davis MJ, Zawieja SD, King PD. Transport and Immune Functions of the Lymphatic System. Annu Rev Physiol. 2025;87(1):151-72. http://dx.doi.org/10.1146/annurev-physiol-022724-104908
5. Winkler F, Venkatesh HS, Amit M, Batchelor T, Demir IE, Deneen B, et al. Cancer neuroscience: State of the field, emerging directions. Cell. 2023;186(8):1689-707. http://dx.doi.org/10.1016/j.cell.2023.02.002
6. Li ZK, Liao JL, Luo MR, Fang SJ, Huang WZ, Zhang DY. Neuro-tumor interactions: Multi-dimensional mechanisms of neurotransmitter regulation in tumor immune evasion and metabolic reprogramming. World J Clin Oncol. 2025;16(10):108954. http://dx.doi.org/10.5306/wjco.v16.i10.108954
7. Saliba J, El-Sabban M, Shaito A, El-Harakeh M, Obeid J, El Hajj H, et al. Cancer metastasis: dynamic hetero-cellular communications between cancer cells and host tissues. Cancerous Cells: Immunobiology of Tumors and Metastasis: Springer; 2025. p. 603-33. https://doi.org/10.1007/978-3-032-00759-9_57
8. Yuan S, Almagro J, Fuchs E. Beyond genetics: driving cancer with the tumour microenvironment behind the wheel. Nature reviews Cancer. 2024;24(4):274-86. http://dx.doi.org/10.1038/s41568-023-00660-9
9. Fang J, Lu Y, Zheng J, Jiang X, Shen H, Shang X, et al. Exploring the crosstalk between endothelial cells, immune cells, and immune checkpoints in the tumor microenvironment: new insights and therapeutic implications. Cell Death Dis. 2023;14(9):586. http://dx.doi.org/10.1038/s41419-023-06119-x
10. Turlej E, Domaradzka A, Radzka J, Drulis-Fajdasz D, Kulbacka J, Gizak A. Cross-Talk Between Cancer and Its Cellular Environment-A Role in Cancer Progression. Cells. 2025;14(6). http://dx.doi.org/10.3390/cells14060403
11. Jhunjhunwala S, Hammer C, Delamarre L. Antigen presentation in cancer: insights into tumour immunogenicity and immune evasion. Nature reviews Cancer. 2021;21(5):298-312. http://dx.doi.org/10.1038/s41568-021-00339-z
12. Shi X. Defining the Causal Contribution of the Gut Microbiota to Cardiomyopathy Pathogenesis as a Basis for Developing Microbiome-targeted Therapies. 2025. https://digitalcommons.unl.edu/foodscidiss/161/
13. Pontis F, Roz L, Fortunato O, Bertolini G. The metastatic niche formation: focus on extracellular vesicle-mediated dialogue between lung cancer cells and the microenvironment. Front Oncol. 2023;13:1116783. http://dx.doi.org/10.3389/fonc.2023.1116783
14. Liu S, Jiang A, Tang F, Duan M, Li B. Drug-induced tolerant persisters in tumor: mechanism, vulnerability and perspective implication for clinical treatment. Mol Cancer. 2025;24(1):150. http://dx.doi.org/10.1186/s12943-025-02323-9
15. Zi R, Zhao X, Liu L, Wang Y, Zhang R, Bian Z, et al. Metabolic-Immune Suppression Mediated by the SIRT1-CX3CL1 Axis Induces Functional Enhancement of Regulatory T Cells in Colorectal Carcinoma. Advanced science (Weinheim, Baden-Wurttemberg, Germany). 2025;12(17):e2404734. http://dx.doi.org/10.1002/advs.202404734
16. Zou Y, Ye F, Kong Y, Hu X, Deng X, Xie J, et al. The Single-Cell Landscape of Intratumoral Heterogeneity and The Immunosuppressive Microenvironment in Liver and Brain Metastases of Breast Cancer. Advanced science (Weinheim, Baden-Wurttemberg, Germany). 2023;10(5):e2203699. http://dx.doi.org/10.1002/advs.202203699
17. Zhou M, Liu H, Hui J, Chen Q, Zhao Y, Wang H, et al. Extracellular Vesicle-Packaged miR-99a Reprograms Fibroblasts to Create an Inflammatory Niche That Drives Colorectal Cancer Metastasis. Cancer Res. 2026;86(1):131-45. http://dx.doi.org/10.1158/0008-5472.can-25-0663
18. Zitti B, Duval F, Wirapati P, Hicham M, Xie Y, Oh J, et al. Positioning and reversible suppression of CCR7(+) dendritic cells in perivascular tumor niches shape cancer immunity. Immunity. 2026;59(1):161-76.e12. http://dx.doi.org/10.1016/j.immuni.2025.11.020
19. Zhou L, Wang M, Guo H, Hou J, Zhang Y, Li M, et al. Integrated Analysis Highlights the Immunosuppressive Role of TREM2(+) Macrophages in Hepatocellular Carcinoma. Front Immunol. 2022;13:848367. http://dx.doi.org/10.3389/fimmu.2022.848367
20. Zhou M, Guan B, Liu Y, Gu Q, Chen W, Xie B, et al. Fibrinogen-like 2 in tumor-associated macrophage-derived extracellular vesicles shapes an immunosuppressive microenvironment in colorectal liver metastases by promoting tumor stemness and neutrophil extracellular traps formation. Cancer Lett. 2025;618:217642. http://dx.doi.org/10.1016/j.canlet.2025.217642
21. Zhou Y, Cheng L, Liu L, Li X. NK cells are never alone: crosstalk and communication in tumour microenvironments. Mol Cancer. 2023;22(1):34. http://dx.doi.org/10.1186/s12943-023-01737-7
22. Zou R, Jiang Q, Jin T, Chen M, Yao L, Ding H. Pan-cancer analyses and molecular subtypes based on the cancer-associated fibroblast landscape and tumor microenvironment infiltration characterization reveal clinical outcome and immunotherapy response in epithelial ovarian cancer. Front Immunol. 2022;13:956224. http://dx.doi.org/10.3389/fimmu.2022.956224
23. Zhou S, Xiao L, Hu L, Zuo F, Wang Y, Fei B, et al. CAFs promote immune evasion in gastric cancer through histone lactylation-mediated suppression of NCAPG ubiquitination. J Transl Med. 2025;23(1):989. http://dx.doi.org/10.1186/s12967-025-07013-0
24. Zhu J, Yang W, Ma J, He H, Liu Z, Zhu X, et al. Pericyte signaling via soluble guanylate cyclase shapes the vascular niche and microenvironment of tumors. Embo j. 2024;43(8):1519-44. http://dx.doi.org/10.1038/s44318-024-00078-5
25. Zhou R, Brislinger D, Fuchs J, Lyons A, Langthaler S, Hauser CAE, et al. Vascularised organoids: Recent advances and applications in cancer research. Clin Transl Med. 2025;15(3):e70258. http://dx.doi.org/10.1002/ctm2.70258
26. Zu Z, Zhang C, Shi J, Chen K, Tang H, Hu K, et al. Single-cell analysis reveals that GFAP(+) dedifferentiated Schwann cells promote tumor progress in PNI-positive distal cholangiocarcinoma via lactate/HMGB1 axis. Cell Death Dis. 2025;16(1):215. http://dx.doi.org/10.1038/s41419-025-07543-x
27. Zhou X, You L, Xin Z, Su H, Zhou J, Ma Y. Leveraging circulating microbiome signatures to predict tumor immune microenvironment and prognosis of patients with non-small cell lung cancer. J Transl Med. 2023;21(1):800. http://dx.doi.org/10.1186/s12967-023-04582-w
28. Zhu Y, Yao Y, Wang Y, Qiu Z, Zhou D, Huang H, et al. Single-cell RNA sequencing unveils enhanced antitumor immunity in colorectal cancer with PD-1 blockade and LINC00673 deletion. Biomark Res. 2026;14(1):16. http://dx.doi.org/10.1186/s40364-025-00888-7
29. Zhu Y, Chen P, Hu B, Zhong S, Yan K, Wu Y, et al. MDSC-targeting gold nanoparticles enhance PD-1 tumor immunotherapy by inhibiting NLRP3 inflammasomes. Biomaterials. 2024;307:122533. http://dx.doi.org/10.1016/j.biomaterials.2024.122533
30. Zhuang J, Shen L, Li M, Sun J, Hao J, Li J, et al. Cancer-Associated Fibroblast-Derived miR-146a-5p Generates a Niche That Promotes Bladder Cancer Stemness and Chemoresistance. Cancer Res. 2023;83(10):1611-27. http://dx.doi.org/10.1158/0008-5472.can-22-2213
31. Zhuang C, Gould JE, Enninful A, Shao S, Mak M. Biophysical and mechanobiological considerations for T-cell-based immunotherapy. Trends Pharmacol Sci. 2023;44(6):366-78. http://dx.doi.org/10.1016/j.tips.2023.03.007
32. Zhu H, Roelands J, Ahmed EI, Stouten I, Hoorntje R, van Vlierberghe RLP, et al. Location matters: spatial dynamics of tumor-infiltrating T cell subsets is prognostic in colon cancer. Front Immunol. 2024;15:1293618. http://dx.doi.org/10.3389/fimmu.2024.1293618
33. Zhu Y, Zhou Z, Du X, Lin X, Liang ZM, Chen S, et al. Cancer cell-derived arginine fuels polyamine biosynthesis in tumor-associated macrophages to promote immune evasion. Cancer Cell. 2025;43(6):1045-60.e7. http://dx.doi.org/10.1016/j.ccell.2025.03.015
34. Zhou Z, Zhang X, Zhu S, Liu W, Guo Y, Xiong S, et al. Crizotinib: A Novel Strategy to Reverse Immunosuppression in Melanoma by Targeting Lactate Transport. MedComm (2020). 2025;6(8):e70286. http://dx.doi.org/10.1002/mco2.70286
35. Zhu J, Wang R, Yang C, Shao X, Zhang Y, Hou J, et al. Blocking tumor-platelet crosstalk to prevent tumor metastasis via reprograming glycolysis using biomimetic membrane-hybridized liposomes. Journal of controlled release : official journal of the Controlled Release Society. 2024;366:328-41. http://dx.doi.org/10.1016/j.jconrel.2023.12.052
36. Zhou Y, Liu Z, Yu A, Zhao G, Chen B. Immune Checkpoint Inhibitor Combined with Antiangiogenic Agent Synergistically Improving the Treatment Efficacy for Solid Tumors. ImmunoTargets and therapy. 2024;13:813-29. http://dx.doi.org/10.2147/itt.s494670
37. Zvirblyte J, Nainys J, Juzenas S, Goda K, Kubiliute R, Dasevicius D, et al. Single-cell transcriptional profiling of clear cell renal cell carcinoma reveals a tumor-associated endothelial tip cell phenotype. Commun Biol. 2024;7(1):780. http://dx.doi.org/10.1038/s42003-024-06478-x
38. Zhou M, Zhou Z, Hu L, Chen S, Meng F, Chen J, et al. Multiplex immunohistochemistry to explore the tumor immune microenvironment in HCC patients with different GPC3 expression. J Transl Med. 2025;23(1):88. http://dx.doi.org/10.1186/s12967-025-06106-0
39. Zhu B, Xiang K, Li T, Li X, Shi F. The signature of extracellular vesicles in hypoxic breast cancer and their therapeutic engineering. Cell communication and signaling : CCS. 2024;22(1):512. http://dx.doi.org/10.1186/s12964-024-01870-w
40. Ziglari T, Calistri NL, Finan JM, Derrick DS, Nakayasu ES, Burnet MC, et al. Senescent Cell-Derived Extracellular Vesicles Inhibit Cancer Recurrence by Coordinating Immune Surveillance. Cancer Res. 2025;85(5):859-74. http://dx.doi.org/10.1158/0008-5472.can-24-0875
41. Zhu Q, Chen X, Duan X, Sun J, Yi W. Targeting glycosylation to enhance tumor immunotherapy. Trends Pharmacol Sci. 2025;46(9):863-76. http://dx.doi.org/10.1016/j.tips.2025.07.013
42. Zuyin L, Zhao L, Qian C, Changkun Z, Delin M, Jialing H, et al. Single-Cell and Spatial Transcriptomics Delineate the Microstructure and Immune Landscape of Intrahepatic Cholangiocarcinoma in the Leading-Edge Area. Advanced science (Weinheim, Baden-Wurttemberg, Germany). 2025;12(7):e2412740. http://dx.doi.org/10.1002/advs.202412740
43. Zhu M, Li N, Fan L, Wu R, Cao L, Ren Y, et al. Single-cell transcriptomic and spatial analysis reveal the immunosuppressive microenvironment in relapsed/refractory angioimmunoblastic T-cell lymphoma. Blood Cancer J. 2024;14(1):218. http://dx.doi.org/10.1038/s41408-024-01199-0
44. Zuo C, Xia J, Chen L. Dissecting tumor microenvironment from spatially resolved transcriptomics data by heterogeneous graph learning. Nat Commun. 2024;15(1):5057. http://dx.doi.org/10.1038/s41467-024-49171-7
45. Zuo Y, Jin Y, Li G, Ming Y, Fan T, Pan Y, et al. Spatial transcriptomic analysis of tumor microenvironment in esophageal squamous cell carcinoma with HIV infection. Mol Cancer. 2025;24(1):54. http://dx.doi.org/10.1186/s12943-025-02248-3
46. Zhou LF, Liao HY, Han Y, Zhao Y. The use of organoids in creating immune microenvironments and treating gynecological tumors. J Transl Med. 2024;22(1):856. http://dx.doi.org/10.1186/s12967-024-05649-y
47. Ai J, Li H, Zhang M, Liu J, Liu L, Sun C. Mechanical Microenvironment in Tumor Immune Evasion: Bidirectional Regulation Between Matrix Stiffness and Immune Cells and Its Therapeutic Implications. Int J Biol Sci. 2026;22(1):280-307. http://dx.doi.org/10.7150/ijbs.121356