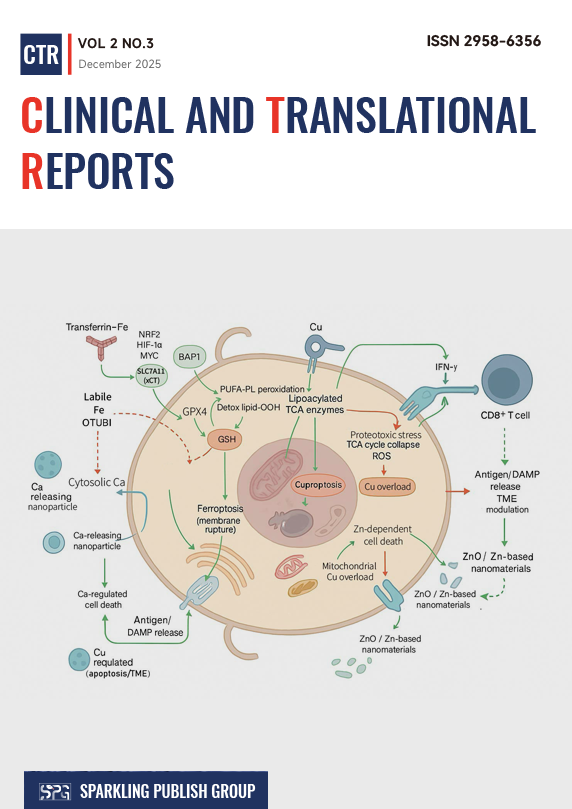
Inflammation is the most visible operational mode of immunity in tissues, translating danger sensing into coordinated vascular, cellular, and metabolic responses that restrict injury and initiate repair. However, the same pathways that protect acutely can become pathogenic when amplification is mis-tuned, tolerance checkpoints fail, or resolution programs stall. This Review synthesizes a circuit-level view of immune inflammation, integrating tissue-encoded cellular networks with modular molecular switches that govern initiation, escalation, and termination. First, it outlines how barrier tissues and tissue-resident immune populations establish local inflammatory set points and explain context-dependent outcomes, exemplified by microbiota-diet interactions that can either support interleukin-22-dependent homeostasis or exacerbate colitis. Then, by describing myeloid circuits as the primary link between perception and systemic consequences, highlighting emerging control layers in RNA metabolism, chromatin remodeling, regulated cell death, and efferocytosis that shape persistence versus regression. Next, it elucidates specific and memory lymphocyte programs that can also lead to tissue damage through tolerance disruption, checkpoint remodeling, or an immunosuppressive microenvironment. Finally, the focus is on the active phase of inflammation resolution, regulated by phased leukocyte degradation, apoptotic cell clearance, and tissue repair, including specific pro-resolution mediators acting as lipid instructions. These mediators complement anti-inflammatory blockade therapies. Across infection, immunometabolic disease, neuroinflammation, fibrosis, and cancer, a unifying principle emerges: durable therapy requires combining selective suppression of maladaptive amplification with restoration of resolution capacity and preservation of protective immune competence.
1. Alfaro S, Acuña V, Ceriani R, Cavieres MF, Weinstein-Oppenheimer CR, Campos-Estrada C. Involvement of Inflammation and Its Resolution in Disease and Therapeutics. Int J Mol Sci. 2022;23(18). http://dx.doi.org/10.3390/ijms231810719
2. Sattler S. The Role of the Immune System Beyond the Fight Against Infection. Advances in experimental medicine and biology. 2017;1003:3-14. http://dx.doi.org/10.1007/978-3-319-57613-8_1
3. Dembic Z. Defending and integrating an organism by the immune system. Scandinavian journal of immunology. 2022;95(5):e13172. http://dx.doi.org/10.1111/sji.13172
4. Zwirner NW, Croci DO, Domaica CI, Rabinovich GA. Overcoming the hurdles of tumor immunity by targeting regulatory pathways in innate and adaptive immune cells. Curr Pharm Des. 2010;16(3):255-67. http://dx.doi.org/10.2174/138161210790170175
5. Palm NW, Medzhitov R. Pattern recognition receptors and control of adaptive immunity. Immunol Rev. 2009;227(1):221-33. http://dx.doi.org/10.1111/j.1600-065X.2008.00731.x
6. Soliman AM, Barreda DR. Acute Inflammation in Tissue Healing. Int J Mol Sci. 2022;24(1). http://dx.doi.org/10.3390/ijms24010641
7. Anderton H, Wicks IP, Silke J. Cell death in chronic inflammation: breaking the cycle to treat rheumatic disease. Nature reviews Rheumatology. 2020;16(9):496-513. http://dx.doi.org/10.1038/s41584-020-0455-8
8. Luo G, Zhang J, Sun Y, Wang Y, Wang H, Cheng B, et al. Nanoplatforms for Sepsis Management: Rapid Detection/Warning, Pathogen Elimination and Restoring Immune Homeostasis. Nano-micro letters. 2021;13:88. http://dx.doi.org/10.1007/s40820-021-00598-3
9. Zrzavy T, Schwaiger C, Wimmer I, Berger T, Bauer J, Butovsky O, et al. Acute and non-resolving inflammation associate with oxidative injury after human spinal cord injury. Brain : a journal of neurology. 2021;144(1):144-61. http://dx.doi.org/10.1093/brain/awaa360
10. Adugna A. Antigen Recognition and Immune Response to Acute and Chronic Hepatitis B Virus Infection. Journal of inflammation research. 2023;16:2159-66. http://dx.doi.org/10.2147/jir.s411492
11. Miceli G, Ciaccio AM, Cuffaro M, Profita M, Tuttolomondo A. Immunology of atherosclerosis as an inflammatory disease: rethinking the dynamic immunoinflammatory activity beneath stability. Expert review of clinical immunology. 2025;21(11):1517-37. http://dx.doi.org/10.1080/1744666x.2025.2575449
12. Zou J, Chassaing B, Singh V, Pellizzon M, Ricci M, Fythe MD, et al. Fiber-Mediated Nourishment of Gut Microbiota Protects against Diet-Induced Obesity by Restoring IL-22-Mediated Colonic Health. Cell host & microbe. 2018;23(1):41-53.e4. http://dx.doi.org/10.1016/j.chom.2017.11.003
13. García LF. Immune Response, Inflammation, and the Clinical Spectrum of COVID-19. Front Immunol. 2020;11:1441. http://dx.doi.org/10.3389/fimmu.2020.01441
14. Zhao X, Wang Y, Wang Y, Gewirtz AT, Zou J. Inulin aggravates colitis through gut microbiota modulation and MyD88/IL-18 signaling. Gut microbes. 2025;17(1):2570425. http://dx.doi.org/10.1080/19490976.2025.2570425
15. Zhou L, Chu C, Teng F, Bessman NJ, Goc J, Santosa EK, et al. Innate lymphoid cells support regulatory T cells in the intestine through interleukin-2. Nature. 2019;568(7752):405-9. http://dx.doi.org/10.1038/s41586-019-1082-x
16. Zheng X, Lei W, Zhang Y, Jin H, Han C, Wu F, et al. Neuropilin-1(high) monocytes protect against neonatal inflammation. Cell Mol Immunol. 2024;21(6):575-88. http://dx.doi.org/10.1038/s41423-024-01157-7
17. Zysset D, Weber B, Rihs S, Brasseit J, Freigang S, Riether C, et al. TREM-1 links dyslipidemia to inflammation and lipid deposition in atherosclerosis. Nat Commun. 2016;7:13151. http://dx.doi.org/10.1038/ncomms13151
18. Zhou Y, Li M, Jin K, Wen M, Qin H, Xu Y, et al. The RNA-binding protein RRP1 brakes macrophage one-carbon metabolism to suppress autoinflammation. Nat Commun. 2025;16(1):6880. http://dx.doi.org/10.1038/s41467-025-62173-3
19. Zhou Y, Yang Z, Wang Y, Dong Y, Wang T, Li Y, et al. Stress granule assembly impairs macrophage efferocytosis to aggravate allergic rhinitis in mice. Nat Commun. 2025;16(1):5610. http://dx.doi.org/10.1038/s41467-025-60920-0
20. Zhou Q, Zhang Y, Wang B, Zhou W, Bi Y, Huai W, et al. KDM2B promotes IL-6 production and inflammatory responses through Brg1-mediated chromatin remodeling. Cell Mol Immunol. 2020;17(8):834-42. http://dx.doi.org/10.1038/s41423-019-0251-z
21. Zhou J, Liu J, Wang B, Li N, Liu J, Han Y, et al. Eosinophils promote CD8(+) T cell memory generation to potentiate anti-bacterial immunity. Signal Transduct Target Ther. 2024;9(1):43. http://dx.doi.org/10.1038/s41392-024-01752-0
22. Zong L, Peng H, Sun C, Li F, Zheng M, Chen Y, et al. Breakdown of adaptive immunotolerance induces hepatocellular carcinoma in HBsAg-tg mice. Nat Commun. 2019;10(1):221. http://dx.doi.org/10.1038/s41467-018-08096-8
23. Zhu T, Xiao Y, Chen Z, Ding H, Chen S, Jiang G, et al. Inhalable nanovesicles loaded with a STING agonist enhance CAR-T cell activity against solid tumors in the lung. Nat Commun. 2025;16(1):262. http://dx.doi.org/10.1038/s41467-024-55751-4
24. Zuo S, Wang B, Liu J, Kong D, Cui H, Jia Y, et al. ER-anchored CRTH2 antagonizes collagen biosynthesis and organ fibrosis via binding LARP6. Embo j. 2021;40(16):e107403. http://dx.doi.org/10.15252/embj.2020107403
25. Zhou Q, Yang YL, Wang JF, Dong YC, Hou J, Guo M, et al. Inflammation-induced Generation of Splenic Erythroblast-like Ter-Cells Inhibits the Progression of Acute Lung Injury via Artemin. American journal of respiratory cell and molecular biology. 2025;73(1):37-48. http://dx.doi.org/10.1165/rcmb.2024-0407OC
26. Zhao Y, Ye X, Dunker W, Song Y, Karijolich J. RIG-I like receptor sensing of host RNAs facilitates the cell-intrinsic immune response to KSHV infection. Nat Commun. 2018;9(1):4841. http://dx.doi.org/10.1038/s41467-018-07314-7
27. Zhou Y, Li M, Xue Y, Li Z, Wen W, Liu X, et al. Interferon-inducible cytoplasmic lncLrrc55-AS promotes antiviral innate responses by strengthening IRF3 phosphorylation. Cell Res. 2019;29(8):641-54. http://dx.doi.org/10.1038/s41422-019-0193-0
28. Zierhut C, Yamaguchi N, Paredes M, Luo JD, Carroll T, Funabiki H. The Cytoplasmic DNA Sensor cGAS Promotes Mitotic Cell Death. Cell. 2019;178(2):302-15.e23. http://dx.doi.org/10.1016/j.cell.2019.05.035
29. Zheng X, Li L, Ma H, Zhu M, Li X, Feng X. Toll-like receptors and their role in the pathogenesis of myasthenia gravis: a comprehensive review. Front Immunol. 2025;16:1624957. http://dx.doi.org/10.3389/fimmu.2025.1624957
30. Zhou W, Wang J, Wang X, Wang B, Zhao Z, Fu J, et al. Degradation of HDAC10 by autophagy promotes IRF3-mediated antiviral innate immune responses. Science signaling. 2022;15(765):eabo4356. http://dx.doi.org/10.1126/scisignal.abo4356
31. Zhu M, Deng G, Xing C, Nie G, Wang RF. BECN2 (beclin 2)-mediated non-canonical autophagy in innate immune signaling and tumor development. Autophagy. 2020;16(12):2310-2. http://dx.doi.org/10.1080/15548627.2020.1839277
32. Zhu C, Zhang W, Liao Y, Jiang R, Cheng L, Wang Y, et al. ERK/Smurf1 regulates non-canonical pyroptosis by prompting Caspase-11 ubiquitination. Cell death and differentiation. 2026. http://dx.doi.org/10.1038/s41418-025-01654-w
33. Zhi Y, Wu X, Chen Y, Chen X, Chen X, Luo H, et al. A novel TWIK2 channel inhibitor binds at the bottom of the selectivity filter and protects against LPS-induced experimental endotoxemia in vivo. Biochem Pharmacol. 2023;218:115894. http://dx.doi.org/10.1016/j.bcp.2023.115894
34. Zou B, Liu J, Klionsky DJ, Tang D, Kang R. Extracellular SQSTM1 as an inflammatory mediator. Autophagy. 2020;16(12):2313-5. http://dx.doi.org/10.1080/15548627.2020.1843253
35. Zhao Y, Zhai L, Qin T, Hu L, Wang J, Zhang Z, et al. Time-Course Transcriptome Analysis of the Lungs of Mice Challenged with Aerosols of Methicillin-Resistant Staphylococcus aureus USA300 Clone Reveals Inflammatory Balance. Biomolecules. 2023;13(2). http://dx.doi.org/10.3390/biom13020347
36. Zhou Y, Liao X, Song X, He M, Xiao F, Jin X, et al. Severe Adaptive Immune Suppression May Be Why Patients With Severe COVID-19 Cannot Be Discharged From the ICU Even After Negative Viral Tests. Front Immunol. 2021;12:755579. http://dx.doi.org/10.3389/fimmu.2021.755579
37. Zuurbier CJ, Abbate A, Cabrera-Fuentes HA, Cohen MV, Collino M, De Kleijn DPV, et al. Innate immunity as a target for acute cardioprotection. Cardiovasc Res. 2019;115(7):1131-42. http://dx.doi.org/10.1093/cvr/cvy304
38. Zhu Y, Cai P, Li Z, Zhang S, Kong WT, Wang H, et al. Transcription factors TCF4 and KLF4 respectively control the development of the DC2A and DC2B lineages. Nature immunology. 2025;26(8):1275-86. http://dx.doi.org/10.1038/s41590-025-02208-5
39. Basil MC, Levy BD. Specialized pro-resolving mediators: endogenous regulators of infection and inflammation. Nature reviews Immunology. 2016;16(1):51-67. http://dx.doi.org/10.1038/nri.2015.4
40. Kim AS, Conte MS. Specialized pro-resolving lipid mediators in cardiovascular disease, diagnosis, and therapy. Adv Drug Deliv Rev. 2020;159:170-9. http://dx.doi.org/10.1016/j.addr.2020.07.011
41. Cole LD, Osborne CM, Silveira LJ, Rao S, Lockwood JM, Kunkel MJ, et al. IVIG Compared With IVIG Plus Infliximab in Multisystem Inflammatory Syndrome in Children. Pediatrics. 2021;148(6). http://dx.doi.org/10.1542/peds.2021-052702
42. Monreal E, Sainz de la Maza S, Fernández-Velasco JI, Natera-Villalba E, Rita CG, Rodríguez-Jorge F, et al. The Impact of Immunosuppression and Autoimmune Disease on Severe Outcomes in Patients Hospitalized with COVID-19. Journal of clinical immunology. 2021;41(2):315-23. http://dx.doi.org/10.1007/s10875-020-00927-y
43. Zuiker E, Serpa G, De M, Liu Y, Wozniak DJ, Gowdy KM, et al. Targeting the MEK1/2 pathway to combat Staphylococcus aureus infection and inflammation in cystic fibrosis. mBio. 2025;16(7):e0077525. http://dx.doi.org/10.1128/mbio.00775-25
44. Vandenabeele P, Bultynck G, Savvides SN. Pore-forming proteins as drivers of membrane permeabilization in cell death pathways. Nature reviews Molecular cell biology. 2023;24(5):312-33. http://dx.doi.org/10.1038/s41580-022-00564-w
45. Zhu B, Sun C, Luo D, Liang Y, Jiang A, Jiang Z, et al. Coptisine Improves Liver Inflammation in Sepsis by Regulating STAT1/IRF1/GPX4 Signaling-Mediated Kupffer Cells Ferroptosis. Phytotherapy research : PTR. 2025;39(9):4308-26. http://dx.doi.org/10.1002/ptr.70063
46. Fan Y, Zhou Y, Zhao J, Zhao Y. Advances in Inhaled Nanoparticle Drug Delivery for Pulmonary Disease Management. FASEB journal : official publication of the Federation of American Societies for Experimental Biology. 2025;39(21):e71191. http://dx.doi.org/10.1096/fj.202502624R
47. Rountree RB, Mandl SJ, Nachtwey JM, Dalpozzo K, Do L, Lombardo JR, et al. Exosome targeting of tumor antigens expressed by cancer vaccines can improve antigen immunogenicity and therapeutic efficacy. Cancer Res. 2011;71(15):5235-44. http://dx.doi.org/10.1158/0008-5472.can-10-4076
48. Bianchi F, Pretto S, Tagliabue E, Balsari A, Sfondrini L. Exploiting poly(I:C) to induce cancer cell apoptosis. Cancer Biol Ther. 2017;18(10):747-56. http://dx.doi.org/10.1080/15384047.2017.1373220
49. Zhu G, Su H, Johnson CH, Khan SA, Kluger H, Lu L. Intratumour microbiome associated with the infiltration of cytotoxic CD8+ T cells and patient survival in cutaneous melanoma. European journal of cancer (Oxford, England : 1990). 2021;151:25-34. http://dx.doi.org/10.1016/j.ejca.2021.03.053
50. Zulu MZ, Sureshchandra S, Pinski AN, Doratt B, Shen W, Messaoudi I. Obesity Correlates With Pronounced Aberrant Innate Immune Responses in Hospitalized Aged COVID-19 Patients. Front Immunol. 2021;12:760288. http://dx.doi.org/10.3389/fimmu.2021.760288
51. Zhou B, Wang DD, Qiu Y, Airhart S, Liu Y, Stempien-Otero A, et al. Boosting NAD level suppresses inflammatory activation of PBMCs in heart failure. J Clin Invest. 2020;130(11):6054-63. http://dx.doi.org/10.1172/jci138538
52. Zhou P, Lai J, Li Y, Deng J, Zhao C, Huang Q, et al. Methyl Gallate Alleviates Acute Ulcerative Colitis by Modulating Gut Microbiota and Inhibiting TLR4/NF-κB Pathway. Int J Mol Sci. 2022;23(22). http://dx.doi.org/10.3390/ijms232214024
53. Zhu W, Li S, Wang C, Yu G, Prausnitz MR, Wang BZ. Enhanced Immune Responses Conferring Cross-Protection by Skin Vaccination With a Tri-Component Influenza Vaccine Using a Microneedle Patch. Front Immunol. 2018;9:1705. http://dx.doi.org/10.3389/fimmu.2018.01705